INTRODUCTION
What if we could prevent cancer before it even starts?
That’s not a hypothetical. That’s not science fiction. That’s the HPV vaccine — and it exists right now, it’s available in India, and millions of families still don’t know about it.
Every year, over 1.25 lakh Indian women are diagnosed with cervical cancer. Around 75,000 of them don’t survive it. These are mothers, daughters, teachers, homemakers — women in the prime of their lives. And the painful truth? A significant portion of these cases could have been prevented with a simple vaccine given during childhood or adolescence.
I’ve sat across from patients who came to me with advanced cervical cancer. I’ve had to deliver news that no doctor wants to deliver and no family wants to hear. And every single time, somewhere in the back of my mind, I think — what if they had known about this vaccine ten years ago?
This article is my attempt to make sure that doesn’t happen to your family.
Let’s break down everything you need to know about the HPV vaccine in India — in plain, honest, empowering language.
 WHAT IS HPV AND HOW DOES IT CAUSE CANCER?
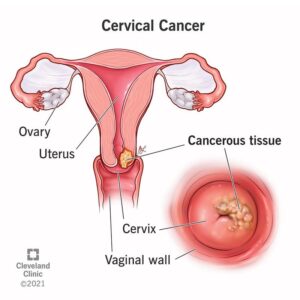
WHAT IS HPV AND HOW DOES IT CAUSE CANCER?
Human Papillomavirus — HPV — is not some rare exotic pathogen. It is, in fact, one of the most common viral infections on the planet. Most sexually active adults will encounter some form of HPV in their lifetime. Many won’t even know it, because the body often clears the infection quietly, without any symptoms at all.
But here’s where it gets serious.
Some strains of HPV are classified as “high-risk.” These strains — particularly HPV 16 and HPV 18 — don’t go away quietly. They linger. They embed themselves in the cells of the cervix, the throat, the anus, or the genitals. And over years — sometimes decades — they quietly reprogram normal cells into cancerous ones.
HPV is responsible for nearly 90% of cervical cancer cases globally. It also drives a significant percentage of anal cancers, oropharyngeal (throat) cancers, penile cancers, and vulvar cancers. This isn’t just a women’s issue. This is a human issue.
Think of HPV as a slow, silent arsonist. It doesn’t announce itself. It just keeps striking matches, year after year, until eventually something catches fire. The good news? We now have a fire alarm — and a fire extinguisher — built into a single injection. https://drsumandas.com/cervical-cancer/
HOW DOES THE HPV VACCINE WORK?
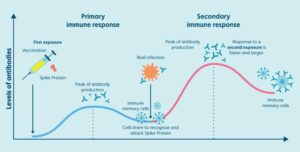
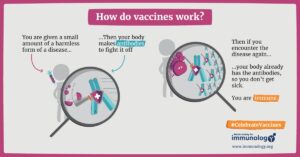
The HPV vaccine doesn’t contain the live virus. It contains virus-like particles — essentially empty shells that look like HPV to your immune system, but have no ability to cause infection. When your body encounters these particles, it mounts an immune response and creates antibodies.
The next time the real virus shows up, your immune system already knows exactly what to do. It neutralizes the threat before it can take hold.
Think of it like this: you’re training your immune system’s army before the battle begins, not during it. That’s what makes this vaccine so powerful — and why timing matters so much.
 Two critical points that often get misunderstood:
Two critical points that often get misunderstood:
The vaccine does NOT treat an existing HPV infection. If you’ve already been exposed to the virus, the vaccine cannot clear it. It won’t reverse pre-cancerous changes, and it won’t cure cancer that’s already developing.
The vaccine PREVENTS future infection. It is a shield, not a sword. Used before exposure, its protection is extraordinary. Studies show up to 98% efficacy against the high-risk strains it covers.
This is why getting vaccinated early — ideally before becoming sexually active — makes such a profound difference.
WHO SHOULD TAKE THE HPV VACCINE?
✅ Ideal Age Group
The sweet spot for HPV vaccination is 9 to 14 years of age. At this stage, the immune system responds with remarkable vigor, producing antibody levels that are two to three times higher than in adults. It’s also well before most individuals have any exposure to the virus.
If your child is in this age group, this isn’t something to debate over chai at the dinner table for six months. It’s something to act on.
✅ Catch-Up Vaccination 
Missed the 9–14 window? You still have options.
Vaccination is recommended up to 26 years of age for both men and women. Between 27 and 45, vaccination is considered on a case-by-case basis — the benefit depends on your prior exposure history, relationship status, and immune health. A conversation with your doctor will help you make the right call.
One important thing I want to address: many parents hesitate to vaccinate their 10 or 12-year-old because the vaccine is associated with sexual transmission. I understand the cultural sensitivity here. But consider this — a seatbelt works best before the accident, not after. We don’t wait for a child to be old enough to drive before we buckle them in. Vaccination works exactly the same way. Protection must come before exposure.
SHOULD BOYS TAKE THE HPV VACCINE?
Absolutely. No hesitation.
This is one of the most common misconceptions I encounter — that the HPV vaccine is “for girls.” It isn’t. HPV is an equal-opportunity virus.

Men can develop HPV-related cancers too: cancers of the throat, anus, and penis. Oropharyngeal cancers driven by HPV are actually rising in India, and they affect men significantly more than women. Boys who are vaccinated protect themselves from these cancers directly.
But there’s another dimension here that’s easy to overlook: herd immunity and community protection. When boys are vaccinated, they are less likely to carry and transmit the virus. This creates a ripple effect of protection — for their future partners, for communities, for the next generation.
Countries like Australia vaccinated both genders aggressively, and they are now on track to functionally eliminate cervical cancer. Eliminate — a word we almost never use in oncology.
Vaccinating only girls is like building a dam on one side of a river. Vaccinating everyone builds the whole dam.
HPV VACCINE DOSE SCHEDULE
| Age Group | Number of Doses | Schedule |
|---|---|---|
| 9–14 years | 2 doses | 0 months, then 6 months later |
| 15 years and above | 3 doses | 0 months, 2 months, 6 months |
Younger adolescents need just two doses because their immune systems respond so powerfully that two doses produce the same antibody levels as three doses in older individuals. This is good news for families — fewer visits, lower cost, and equally strong protection.

One practical note: don’t abandon the schedule midway. A single dose provides partial protection, but you need to complete the recommended course for full immunity. If you’ve had your first shot and life got busy, don’t assume the series has lapsed — speak to your doctor. In most cases, you can pick up where you left off.
HPV VACCINE COST IN INDIA (2026)
| Vaccine | Approximate Cost Per Dose |
|---|---|
| Cervavac (India’s own vaccine) | ₹1,500 – ₹2,000 |
| Gardasil (4-valent) | ₹2,500 – ₹4,000 |
| Gardasil 9 (9-valent) | ₹7,000 – ₹10,000 |
Cervavac — developed by the Serum Institute of India — is India’s first indigenously manufactured HPV vaccine, approved by the Drugs Controller General of India. It covers the two highest-risk HPV strains (16 and 18) responsible for the majority of cervical cancers. For most Indian families, Cervavac offers excellent protection at a much more accessible price point.
Gardasil 9 covers nine HPV strains and offers broader protection, including against strains that cause genital warts. For families who can afford it, this wider coverage is an advantage. But it’s important to understand: even Cervavac, covering just strains 16 and 18, prevents the cancers that matter most.
A reassuring development: several state governments have now begun offering the HPV vaccine free of cost for adolescent girls through school health programs. Check with your local government health office or school administration — your daughter may already be eligible.
The real cost conversation isn’t rupees, though. It’s this: the cost of treating cervical cancer — financially, emotionally, physically — is immeasurably higher than the cost of prevention.
https://www.pib.gov.in/PressReleasePage.aspx?PRID=2233632®=3&lang=1
WHY DOES THE VACCINE WORK LESS IN OLDER WOMEN?
This is a fair and important question — and it deserves a straight answer.
The vaccine’s effectiveness decreases with age primarily because older individuals are more likely to have already been exposed to HPV. Since the vaccine prevents new infections rather than treating existing ones, someone who has already encountered the virus gains less benefit.
That said, “less benefit” doesn’t always mean “no benefit.” HPV has multiple strains, and vaccination can still protect against strains you haven’t been exposed to. This is why vaccination is still considered beneficial — on a case-by-case basis — up to age 45.
Here’s the analogy I use with patients: imagine locking your front door after you’ve already left for work. Doesn’t help for the day you’ve already started, but it still protects you on every day that follows.
If you’re over 26 and wondering whether it’s too late, the answer isn’t a flat yes or no — it’s a conversation worth having with your doctor, one tailored to your individual history and risk profile.
SIDE EFFECTS OF HPV VACCINE
Let me be clear and direct here, because misinformation about vaccine side effects is everywhere — and it costs lives.
The HPV vaccine is safe. It is one of the most extensively studied vaccines in the history of modern medicine, with safety data from hundreds of millions of doses administered globally over nearly two decades.
Common side effects (usually mild and short-lived):
- Pain, redness, or swelling at the injection site
- Low-grade fever
- Mild fatigue or headache
- Occasionally, dizziness immediately after injection — which is why doctors typically advise sitting for 15 minutes post-vaccination
Rare:
- Allergic reactions — extremely uncommon, and always manageable when vaccination is done in a clinical setting
The stories circulating on social media linking the HPV vaccine to serious neurological conditions, infertility, or autoimmune diseases have been investigated rigorously by health authorities worldwide — the WHO, the CDC, the CDSCO in India — and consistently found to be without scientific basis.
Vaccine hesitancy fueled by misinformation is not caution. It’s a risk in the other direction.
SHOULD YOU TAKE THE HPV VACCINE?
Let me answer this the way I would if you were sitting across from me in my clinic, asking me face-to-face.
If you have a child between 9 and 14 years old, yes — vaccinate them. Full stop. This is one of the clearest, most evidence-backed preventive health decisions you can make for your child’s future.
If you’re a young adult between 15 and 26 who hasn’t been vaccinated, yes — it’s not too late. Speak to your doctor this week.
If you’re between 27 and 45, the answer is “probably, depending on your situation” — which means it’s worth a 10-minute conversation with your gynecologist or primary care physician.
What makes the HPV vaccine unique in all of medicine is this: we are talking about a vaccine that prevents cancer. Not treats cancer. Not manages cancer. Prevents it. In the history of oncology, this is a gift we’ve almost never been given. We should use it.
FINAL THOUGHT
In medicine, most of our work is reactive. Cancer appears, we fight it. Disease strikes, we respond. We are warriors of the aftermath.
But with HPV vaccination, we have something different — a rare, precious, scientifically proven chance to intercept cancer before it begins. To protect your daughter, your son, your family from a diagnosis that changes everything. To rewrite a future that would otherwise be written in hospital corridors and chemotherapy chairs.
That is not just medicine.
That is one of the most powerful acts of love a parent can perform.
Don’t wait. Talk to your doctor. Get vaccinated.
A NOTE ON CONTINUING THE CONVERSATION
Cervical cancer is just one part of the HPV story. If you found this article useful and if you’re a parent, caregiver, or patient who still has questions after reading this, reach out. That’s exactly what this space is for. Subscribe and Share if you find value.
Dr. Suman Das is a Radiation Oncologist at Apollo Cancer Center, Visakhapatnam, and the creator of The Healing Monk — a platform dedicated to making cancer medicine accessible, honest, and human.
Subscribe to drsumandas.com for evidence-based health insights written in plain language.












11 Comments
Prof Dr A V Subhash
April 7, 2026Sir,
you managed to take a complex topic & make it incredibly accessible. Evidence based & most importantly reassuring for parents & young adults. The proactive approach you outlined is essential for protecting the next GENERATION from.preventable cancers.
Dr Suman Das
April 8, 2026Thank you sir. Its the need of the hour.
Chetan Raju
April 8, 2026Suman ji,
I really appreciate how clearly you explained the importance of the HPV vaccine. It’s encouraging to see more awareness being created around prevention rather than just treatment.
Dr Suman Das
April 8, 2026Thank you. All children should be vaccinated to avoid a catastrophe in future.
Bheem srinivas
April 8, 2026I’m extremely grateful for the insightful information, sir . It has clarified several aspects and I’ve already shared it with others . While ‘thank you’ seems inadequate, I deeply appreciate the time and effort you took to share this with me
Dr Suman Das
April 8, 2026Thank You Srinivas. I hope it helps the readers and more and more people do vaccination for their children.
Palak
April 8, 2026What a lovely article,thanks Doctor for sharing this
Dr Suman Das
April 8, 2026Thank you dear.
Prasad
April 8, 2026Thankyou sir,
I am 40 ,male ,which vaccine (gardacil4 or gardacil 9)can I take?
Prasad
April 8, 2026Thankyou sir,
I am 40 ,male ,which vaccine (gardacil4 or gardacil 9)can I take?
I am from kakinada
Dr Suman Das
April 8, 2026Usually efficacy is less if already exposed to the virus. Gardasil 9 has more coverage of strains of the virus, can take that.